Hearing Voices Linked to Self-Talk Brain Glitch

Nadia Chen

For decades, the experience of hearing voices has been one of psychiatry's most profound mysteries. Often associated with schizophrenia, these auditory hallucinations can be terrifying and isolating. New research is now providing the clearest biological evidence yet for what may cause this phenomenon.
The key lies in a fundamental brain process called corollary discharge. This is the brain's way of tagging its own internal commands. When we move or speak, a prediction signal is sent to sensory areas, telling them to dampen their response. For the first time, scientists have measured this signal going awry during inner speech in people who hallucinate.
This disruption suggests a "brain glitch" where the mind fails to recognize its own thoughts. Instead of being identified as internal, the inner voice is processed as if it belongs to someone else. This discovery moves us from theory toward tangible biology, offering a potential window for earlier intervention.
The Voice in Your Head
Inner speech is your brain's internal monologue, the voice that narrates your conscious experience. It's the stream of thoughts that plans your day, rehearses conversations, or reads these words in your mind. For most, this internal monologue is a constant, quiet companion. The brain expertly manages this activity by predicting the sensory consequences of our own thoughts.
This prediction mechanism is crucial for a stable sense of self. It allows us to distinguish between actions we initiate and events that happen to us. When you speak aloud, your auditory cortex is less responsive to the sound of your own voice. The brain anticipates it and turns down the volume, so to speak.
This same dampening should occur with imagined speech. Your brain knows you are generating the thought internally. New research confirms this is exactly what happens in neurotypical individuals. But in schizophrenia, this elegant system appears to break down.
Listening to Silent Speech
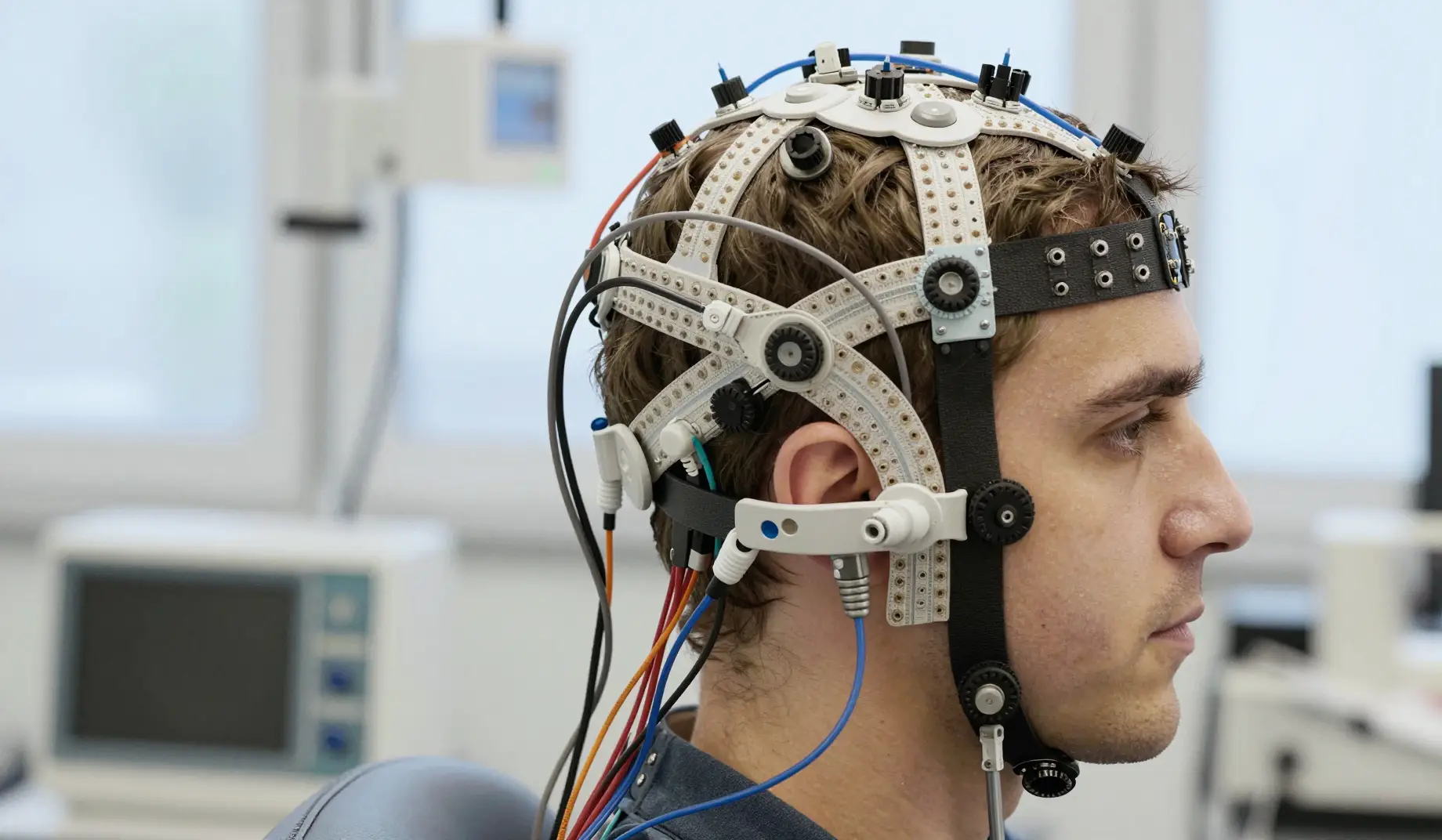
Testing a theory about private inner speech required an ingenious method. Researchers at UNSW Sydney used electroencephalography (EEG) to measure brainwaves during a carefully designed task. Participants were fitted with caps containing sensors that detect electrical activity from the brain's surface.
Participants heard spoken syllables through headphones. On cue, they were told to mentally rehearse saying one of those syllables without making a sound. Crucially, the external sound they heard sometimes matched their inner speech and sometimes did not. The brain's reaction to this match or mismatch holds the key.
In neurotypical participants, auditory cortex activity decreased when the mentally rehearsed syllable aligned with the external audio. The brain had anticipated the sensory signal and dampened its neural firing in response. This is the neural signature of recognizing your own mental action. The experiment provided a direct way to eavesdrop on the brain's self-monitoring system.
The study involved three distinct groups for clear comparison. One group had schizophrenia with recent auditory hallucinations. A second group had schizophrenia diagnoses but hadn't heard voices recently or ever. The third group was neurotypical with no schizophrenia history. This design allowed scientists to isolate the effect specific to active hallucinations.
When Prediction Fails
The results revealed a striking reversal in brain activity. For healthy participants, the expected suppression effect was clear. Their auditory cortex showed reduced activity when their inner speech matched the external sound. This is the brain correctly saying, "I made that."
For participants currently experiencing auditory hallucinations, the pattern flipped entirely. Their brain activity ramped up when their inner speech matched the external sound. Their sensory processing areas reacted more strongly, as if surprised by the coincidence. This suggests the brain did not send an effective prediction signal.
It perceived the match as an unexpected external event. The inner thought was not recognized as self-generated. This neural confusion could be the root of the voice-hearing experience. The person's own cognition feels alien and arrives as an external voice.
The schizophrenia group without recent hallucinations showed an intermediate response. Their suppression effect was weaker than healthy controls but not reversed like the hallucinating group. This gradient hints that the glitch may exist on a spectrum, correlating with symptom severity.
From Theory to Biomarker
This work provides strong empirical support for a long-held theory. For over fifty years, clinicians have proposed that hallucinations might be misattributed inner speech. The private nature of thought made it nearly impossible to test directly. This EEG methodology finally offers an objective measurement.
The disrupted corollary discharge is a compelling candidate for a biological marker, or biomarker. Psychiatry urgently lacks such objective tests. Diagnoses rely on observed behaviors and reported symptoms. A measurable brain signal could revolutionize the field.
A reliable biomarker could aid in early detection. It might identify individuals at high risk of psychosis before full-blown symptoms appear. Early intervention is closely linked to better long-term outcomes. This could shift treatment toward prevention.
It also offers a new target for therapeutic development. Treatments could aim to correct or compensate for this faulty predictive signal. Understanding the mechanism is the first step toward designing more effective interventions. This moves the focus from just managing symptoms to addressing a root cause.
A Path Forward
The implications of this research extend beyond schizophrenia. The brain's self-monitoring system is fundamental to consciousness. Its failure might contribute to symptoms in other conditions where agency is distorted. Studying this glitch provides a window into how we construct our sense of reality.
Future research will track this brain signal over time. Scientists want to see if it can predict who will develop psychosis. Longitudinal studies following at-risk youth are the logical next step. The goal is a predictive tool for clinicians.
There are also questions about specificity. Is this glitch unique to schizophrenia with auditory hallucinations? Or does it appear in other psychiatric or neurological disorders? Comparing across diagnostic categories will be essential. The answer could refine our understanding of mental illness itself.
This discovery bridges the subjective and the biological. It connects a deeply personal, often distressing experience to a measurable neural process. For those who hear voices, it validates their reality as a neurobiological event, not just a psychological one. It frames the symptom as a breakdown in a specific circuit, opening new avenues for hope.
Sources
- Journal PublicationOriginal peer-reviewed research published in Schizophrenia Bulletin describing the EEG study of corollary discharge dysfunction in patients with schizophrenia.
